Like birthdays and anniversaries, November 12, 2017 will forever be a date etched in my memory. My daughter, Sophia had a fever and fell asleep on my husband. It was so sweet that I took a picture. Little did I know this picture would represent the start of a long journey for our family, her headaches, confusion, anger, our countless trips to doctors’ offices, the Emergency Room and eventually, hospitalization.

For the first seven years of her life, Sophia was a happy and healthy little girl. After her fever that November day, she started experiencing debilitating headaches and changes to her personality. She would have angry outbursts and spontaneously start crying. She was confused and forgetful.
In the weeks that followed, her symptoms were dismissed by doctors as a sinus infection or migraines. My husband and I knew it was something more and fought hard to get her the care she needed. She was hospitalized at one point and given anti-migraine medicine and steroids. In hindsight, she improved each time she was on steroids, but the effects were short-lived once her taper was finished.
Sophia missed numerous days of school during this time. On a day she was going back, she had a massive absent seizure in our living room. Her entire body froze, and her eyes became fixated on the ceiling. Somehow, I knew she was having a seizure, but didn’t think to call 911. We carried her to the car and drove to the nearest hospital 10 minutes away.
Watching our little girl seize in the ER while doctors frantically worked to stabilize her was terrifying. The sheets were soaked with blood from failed IVs. She seized off and on for what seemed like an eternity. As soon as she was stable, she was transported to a larger hospital. I realized the severity of the situation when the critical care team rode with us for the 20-minute ambulance trip.
Sophia was in and out of consciousness for the next few days. An MRI confirmed encephalitis, but they could not determine the cause. The head of the PICU sat us down and recommended we transfer to one of the teaching hospitals in the area. I will always be grateful to him for his candor about the complexity of her condition and his incredible empathy.
We embarked on another ambulance ride, with the same critical care team, this time to an even bigger hospital. We were met with a revolving door of specialists; Hematologists, Oncologists, Infectious Disease Specialists, Neurologists, Rheumatologists, all trying to determine the cause of her encephalitis. We racked our brains in answering their questions. Could it be the alligators we fed on vacation? Or the beach we went to after a hurricane? Was she scratched by an animal or bitten by a tick?
Sophia continued in the throes of encephalitis, becoming extremely angry and agitated. Her arm was strapped to a board, so she wouldn’t rip out her IV. She was violent; punching doctors, EEG techs and the IV team. I’m certain her screaming woke up the entire floor at night. She developed facial tics and auditory hallucinations. One night, her oxygen levels were dangerously low, and her PICU nurse and I spent the entire night watching the monitors, holding oxygen by her face.
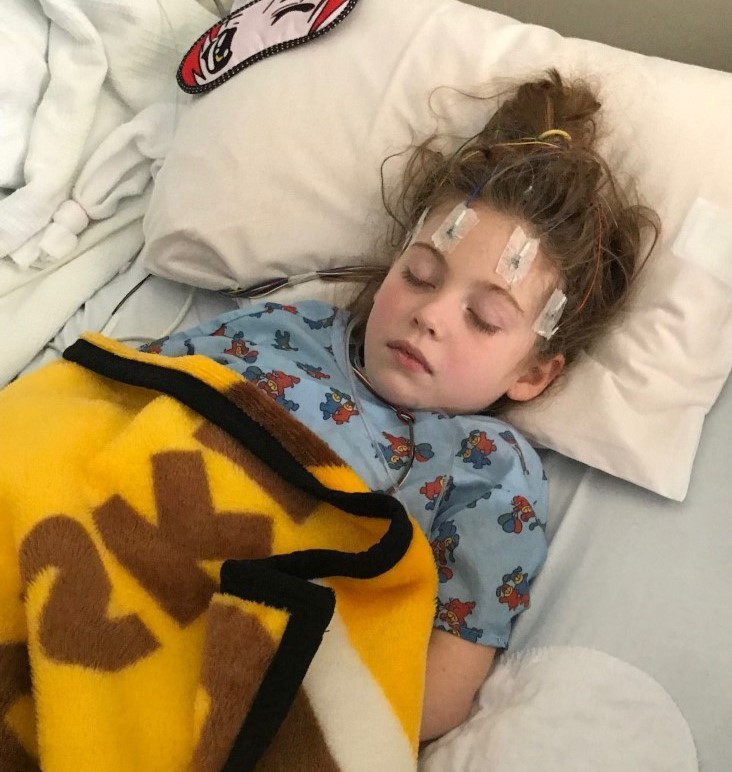
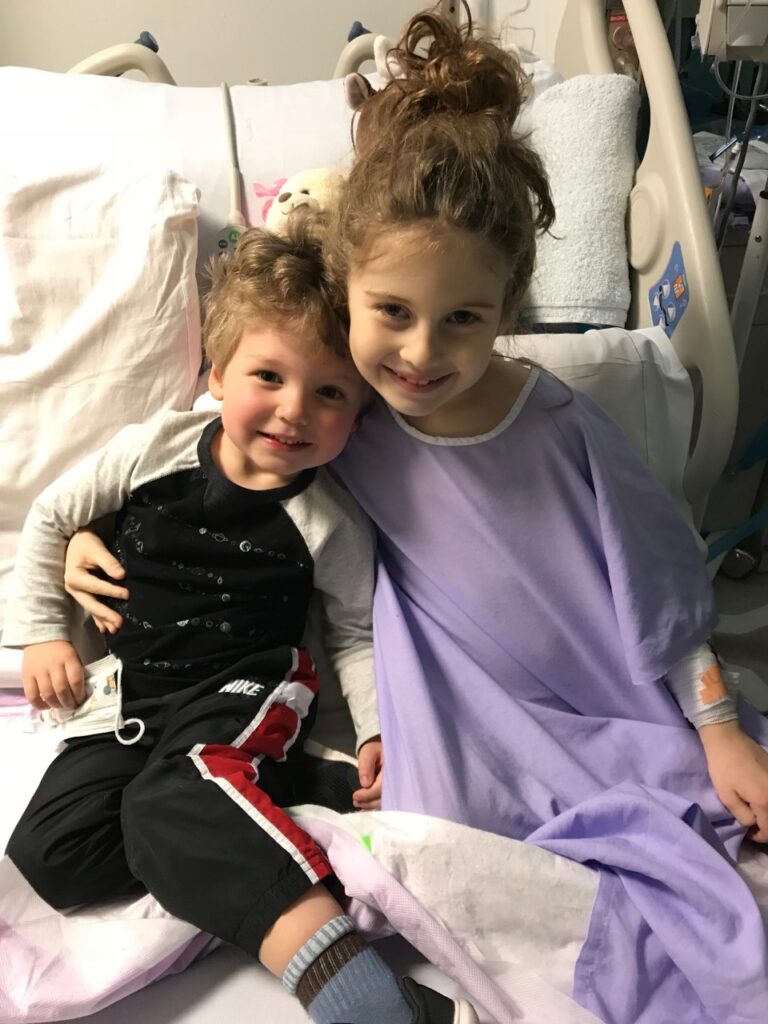
After a few days of IV steroids and IVIG, Sophia began to wake up. The excitement that she was starting to get better was tempered by the realization we had lost part of our little girl. She had absolutely no memory of her little brother and had lost a significant amount of her vocabulary. It was devastating. However, over the next few days, she made an amazing recovery and was getting closer to the Sophia we knew before this illness.
Her diagnosis at discharge was Seronegative Autoimmune Encephalitis. However, two days after she was discharged, she experienced Optic Neuritis. She was hospitalized again for another round of IV steroids. Thankfully, her doctors were aware of MOGAD and immediately sent her blood to the Mayo Clinic for MOG Antibody testing. A week later, we received her positive test result.
Sophia was diagnosed with MOGAD within three months of initial symptoms. Her case exemplifies being in the right place at the right time and I am forever grateful to her doctors for that. For many MOGAD patients, the diagnosis journey is much longer. Sophia has made nearly a full recovery, her brain lesions have healed and while she still struggles with vision issues, she tests at 20-20. She has remained fairly stable the past few years and continues to take immunosuppressants to keep the MOG antibody at bay.

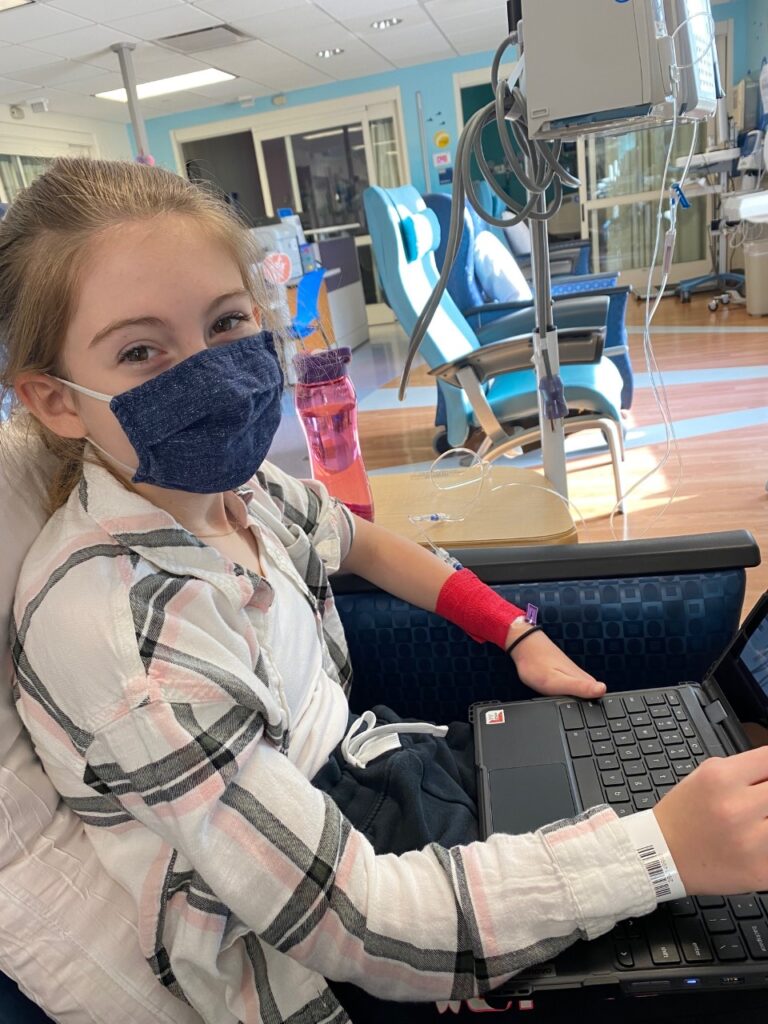
Our lives have been forever changed. There will always be a line representing Sophia’s MOGAD diagnosis in our family’s timeline. During this journey, we have met incredible people who are part of the MOGAD community. I am a Board Member and Pediatric Ambassador for The MOG Project. Working with this amazing organization has enabled me to channel my anxiety, frustration, and fear over Sophia’s diagnosis into something productive. I am so proud of the resources, support, and advocacy we provide for MOGAD patients and their caregivers every day.
Sophia continues to face her challenges head-on with strength and perseverance. She is funny, artistic, beautiful, a talented musician and an amazing person. Our family hopes that over time, MOGAD becomes a smaller part of our life. For now, we’ll face the challenges together, with courage, strength, a few tears, and a lot of love.


By Jennifer Gould, Director of Pediatric Research Advocacy and Executive Board Member of The MOG Project



Jen, this is such a beautiful, pull-on-your-heart-strings post. I still can’t imagine what it was like for you and Mark to live through those initial weeks in the hospital. Sophia is definitely a lucky girl in many ways!
Bless her heart and your whole family! ❤️
Thank you so much for sharing. My 9 year old son (now 10, almost 11) started off very similar.
In early October 2020 on three occasions my son Niko complained of a headache and eye ache on the left. But he would mention it so brief and then would go back to his playful self. So I didn’t think much of it but made a mental note to be aware. This was partly because Niko was incredibly heathy with no health issues.
A couple days before Halloween of 2020, my son started exhibiting unusual characteristics. He was lethargic, lost interest in eating, and didn’t even want to play his video games. He started to become very snuggly and slept for nearly two days straight. At first I thought maybe a growth spurt? Perhaps a new tooth coming in? Perhaps a sinus infection?
I started researching/googling all the possible scenarios. It was confusing because initially his symptoms were mild enough to be confused with other symptoms.
I realized something was off when it was Halloween and he opted to not to partake in any Halloween festivities with his friends and he just wanted to sleep.
Sudden panic started to kick in but I worked hard to not show it. Over the next two days I took Niko to urgent care on 10/31/20 and his primary doctor on 11/2/2020. Both visits determined him to be fine but during his visit on 11/2/2020 there was a brief moment when Niko appeared as if he wanted to go to sleep. At this point the doctor point blank asked Niko if he wanted to sleep as if he did he would need to go the hospital. Suddenly Niko perked up. At this point the doctor and I agreed to closely monitor Niko over the next two days. Little did I know this was the start of our incredibly scary, isolating journey.
Almost 17 months ago (11/4/2020) my son woke up crying…he was barely unable to see and had an unsteady gait. I immediately called his doctor and we coordinated at ZOOM meeting. Upon the doctor coming on, it was very evident how much Niko had declined since his visit two days prior. Niko was crying, feverish, unable to communicate clearly, and constantly rubbing his head and neck. Both the doctor and I immediately suspected meningitis and I was told to take Niko to ER immediately. Before I even had a chance to gather my belongings…Niko — a child who doesn’t like going to doctors — ran to the car barefoot barely able to stand.
We made our way to the ER at Valley Medical Hospital where we spent the next several hours as Niko underwent numerous tests including lumbar punctures, COVID and viral and bacterial tests. Everything was coming back clear and negative but at the same time we could see Niko cognitively deteriorating more and more as the day went on…which perplexed the doctor attending to Niko. I could also tell this was personal for the doctor as he told me he had a son the same age and it struck him as if Niko was his son.
After hours of research and investigative efforts, I learned that the ER doctor had been in touch with Seattle Children’s for guidance. Next thing I knew an ambulance crew was at our bay door to transport Niko to Seattle Children’s.
Niko was admitted to Seattle Children’s on 11/4/2020 and after numerous tests and MRI’s it was determined Niko had ADEM, Transverse Myelitis, and Optic Neuritis. Niko suddenly lost his vision entirely and ability to swallow and speak. Next Niko ended up in a coma and was intubated. A few days later we learned his conditions was a result of a diagnosis known as MOGAD.
The series of angst, confusion and begging questions began. What is ADEM? what is TM? what is ON? What is MOGAD? What caused all this? What must we do to cure and save him? “Help! I am begging you…” I cried and pleaded at the several different specialists.
Over the next few months after several treatments with several MRI’s, six rounds of PLEX, five days of high dose of methylprednisolone, six months of Cytoxan with dexamethasone (because I learned dexamethasone penetrates the BBB whereas methylprednisolone does not. so I asked for the switch) and monthly IVIG (17 to date as of this writing)…15 months into Niko’s diagnosis, his MOGAD finally became negative and his TM cleared! My son also received his first medically stable MRI with no new brain lesions!
While Niko is currently still immobile and non-communicative, he is finally starting to regain purposeful movement (so much so he keeps pulling out his NG tube and yanking on his trach) and he is visually tracking. Though we’re still not sure to what extent as he is still non-communicative.
The road ahead still faces so many MANY unknowns and I find myself struggling daily on how to navigate my fears, frustration, depression, sadness and most of all my guilt. I ache to leave my job so I can focus on Niko but not sure if it’s realistic financially.
I ask myself frequently…if I had recognized and done something sooner could I have prevented this? Had I not gotten him the flu vaccination two weeks before symptoms started surfacing would we be in this situation? This thought peered in my mind because he had gotten the flu vaccination in his left deltoid and his subtle symptoms started presenting in his left eye and left temple areas within just two weeks. As much as I didn’t want to admit it, the sinking feeling that the flu vaccination and the timing and coincidences were too great to ignore.
At first I was told the vaccination was likely not the cause but then after two brain biopsies, a leg muscle biopsy (to rule out mitochondrial disorders), four infectious disease work-ups and four genetic work-ups (two via UW Pathology and two via Prevention Genetics), thankfully all the results came back clear/negative. It was at that point that it was acknowledged that the flu vaccination may indeed be the cause of Niko’s condition. As a result his primary neurologist filed a VAERS report.
I realize the condition varies from person to person but I am desperate to connect with someone who understands how isolating this experience is. I am eager for guidance on how to channel this experience emotionally and possibly even professionally… as not only do I want to advocate for Niko’s full recovery but to spare other families the sense of isolation, as well as bring awareness on ADEM/TM/ON/MOGAD.
Just know…Niko is our everything and we will never give up on a hopeful full recovery.
Niko has been an inpatient at Seattle Childrens for almost 17 months (partly due to home nursing shortages) and we’re starting the steps to bring him home hopefully by summer 2022.
Thank you for taking the time to read this message.
God bless,
Sherrie (from iPhone)
Sherrie, please consider joining The MOG Project’s support group for parents. It’s under the Community tab at the top of the website. Dawn and Brian are wonderful and run the group. We also have a very active Facebook community with many parents and caregivers (MOG Antibody/Anti MOG Support and Info). Your son’s story breaks my heart. You sound like an amazing, strong mom. I hope you can bring him home soon.
Thank you for sharing this Jen. My heart goes out to you and your family. I didn’t realize the extent of what you went through and Sophia for that matter. So glad they figured it out and that your persistence paid off. Love you guys!
Comments are closed.